
The refractive index of the natural crystalline lens is 1.4. The refractive index is a measure of the bending of a ray of light, calculated by the ratio of the velocity of light within a vacuum to the velocity of light within the material. 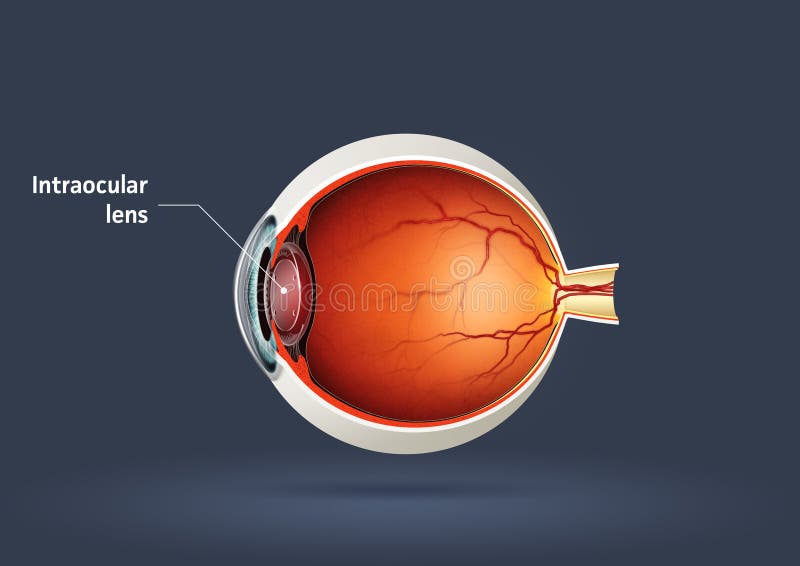
IOLs are manufactured with a goal glass transition temperature below the physiologic body temperature of 37☌ and normal room temperature because materials with a glass transition temperature above 37☌ or normal room temperature would not unfold at physiologic body temperatures or at room temperature. The glass transition temperature of a polymer is the temperature at which the polymer changes from a rigid, solid-like glassy fluid to a softer, rubber-like fluid. A polymer appears solid at lower temperatures because its chains move slowly, whereas it transitions to a viscous material at higher temperatures due to increased energy and molecular mobility. The fluidity of polymers changes with temperature. This is likely because once water enters the material, it interacts with hydrophilic groups and therefore does not collect in microvacuoles. Increasing a material’s hygroscopy reduces the common postoperative appearance of glistenings, which are small fluid-filled microvaculoes that appear after IOL implantation. Hygroscopy is the ability of a material to absorb and hold water (also known as a lens material's equilibrium water content). Large contact angles define hydrophobic materials, whereas smaller angles define hydrophilic materials. The contact angle measures the degrees between the material’s surface and water droplet’s surface. Īn IOL material surface may be hydrophilic or hydrophobic, measured by photographing a water droplet placed onto the material surface. Uveal biocompatibility refers to how well an IOL is tolerated in the eye without causing immunogenic responses of the anterior choroid, ciliary body, and iris. Capsular biocompatibility is determined by direct contact of the IOL with remnant lens epithelial cells (LECs), which may lead to adherence and anterior capsule opacification (ACO) and posterior capsule opacification (PCO). IOL materials must also block ultraviolet rays, be optically transparent, and have a high refractive index. īiocompatibility is defined as the capability of an implanted IOL material to remain optically functional in vivo without causing significant adverse responses such as anaphylaxis, inflammation, necrosis, rejection, thrombosis, or tumorigenesis. 
Accommodation, contrast sensitivity, emmetropization, and visual acuity are all affected by chromatic aberration. In pseduophakic eyes, however, various IOL materials determine LCA, with Abbe numbers ranging from 37-55. Moreover, chromatic dispersion does not vary significantly from one person's eye to another. The human visual system exhibits spherical refractive errors of 2.5D within the visible spectrum however, the phakic human eye is well adapted to this longitudinal chromatic aberration (LCA) due to compensatory mechanisms, including blue-light filtering capabilities of the lens and macula. The Abbe number of the natural crystalline lens is 47. As the refractive index increases, the Abbe number decreases. The Abbe number is a measure of an optical material's chromatic dispersion, with higher values representing lower chromatic dispersion, and better optical quality. These properties contribute to visual quality. IOL materials can be classified using various properties they possess including abbe number, biocompatibility, hydrophobicity, hygroscopy, glass transition temperature, and refractive index. These IOL materials contain distinct physical and optical properties, with unique advantages and disadvantages. While PMMA was the first material to be used in IOL implantation, technological advances have brought about silicone and acrylic lenses, which are foldable and therefore, more applicable with the advent of small-incision, phacoemulsification-assisted cataract surgery. A variety of IOL materials are currently available, including collamer, hydrophobic acrylic, hydrophilic acrylic, PEG-PEA/HEMA/Styrene copolymer, polymethylmethacrylate (PMMA), and silicone. Since the introduction of the first modern IOL in 1949, IOL materials and designs have evolved to encompass medical needs. Intraocular lenses (IOLs) are commonly implanted after surgical removal of a cataractous lens. 3.4 PEG-PHS/HEMA/Styrene (PHS) Copolymer.
0 Comments
Leave a Reply. |
 RSS Feed
RSS Feed
